|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
In order to be sure of progress in motor rehabilitation, video documentation and regular measurements are helpful and they are a must for any scientific work to be done. In the latter case it is also important to have comparable assessments. SCI. FRANKEL scale is very practical since it gives a quick and simple functional assessment, but is not sensitive enough to measure progress in walking either, FIM does not even distinguish between locomotion with
and without wheel For these reasons and to adopt to the progress in
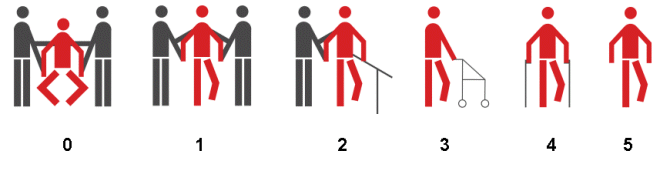
walking we may achieve with LB therapy we have suggested 2 new assessments. Functional Classes (0 - 5 ) for locomotion: Minimum distance: 5 m Dependent: 0: not capable of walking even with help from two therapists; 1: capable of walking with moderate help from 2 therapists; 2: walking at the railing with one therapist. Independent: 3: rollator or reciprocal frame; 4: Regular crutches; 5: without devices. The classes graphically: Functional Classes SCI: The amount of voluntary muscle activity may be evaluated
from the force and range of single joint movements evokable upon
verbal command in defined resting positions (horizontal and sitting),
avoiding readily evokable spastic extension or flexion patterns
(Kendall et al.,1971). Under these rating conditions, values were
defined as follows: 0=no muscle contraction visible or palpable;
1=muscle contraction visible and/or palpable, no movement of limbs;
2=some joint angle movement with passive support by the therapist
balancing gravity; 3=full range of joint angle movement against
gravity; 4=full movement plus maintenance of position against moderate
applied resistance; 5=like 4, against maximal applied resistance.
Values in between were allowed and valued as 1/2 points. Cumulated
Muscle Index: Glutaeus maximus, Glut.med. and min., Iliopsoas, Sartorius,
Quadriceps fem., Ischiocrurales, Tibials ant., Triceps surae. ASSESSMENTS for SCI persons 1.Walking capability: FIM-walking (not locomotion
or stairs), EU- At the beginning and end of therapy and at 6 and 12
months: PLEASE NOTE: Definition of the treatment given to
the control group is obviously important. It appears that more and
more researchers (e.g. Nilsson et al 2001; Kosak et al 2000) choose
to give the control group a very intensive locomotor training, which
was not done a few years ago, when non-ambulating patients were
rather discouraged to consider walking as a primary goal rather
than to try the borders. We realise that this shift in attitude
very much comforts our new dogma: If one wants to walk again one
needs to exercise upright walking (Wernig et al 1991, 1992). If
our previous work has contributed to this dramatic shift in therapeutic
approach, much has already been achieved. However, it blurs the
definitions of such trials. Now not any longer intensive upright
walking (on the treadmill) is compared to "conventional"
physiotherapy (with limited stress on training of walking for non-ambulating
patients), but different ways to train upright walking. This shift
then necessarily causes a shift in the scientific questions to ask
from a trial. Rather than asking whether LB therapy is superior
to conventional physiotherapy, the question now is for the efficacy
of the therapeutic approach: This includes therapy time, amount
of effort therapists need to put into walking the patient (walking
on the treadmill with the patient secured by a harness and body
weight supported versus walking over ground also with non-ambulating
patients), number of therapists necessary to support the training,
time to reach independent ambulating and so on. 7.2 Hemiplegia 7.2.1 Functional Ambulation Category (FAC):
Holden et al 1984, Phys Ther 64, 35-40. 7.2.2 Motricity Index to test motor strength (both sides)(Demeurisse et al 1980, Eur Neurol 19, 382-389.): Pinch grip, elbow flexion, shoulder abductíon, ankle dorsiflexion, knee extension, hip flexion. 7.2.3 Scientific trial For later stratification:
|
 Assessments
of motor capability in SCI and stroke patients
Assessments
of motor capability in SCI and stroke patients